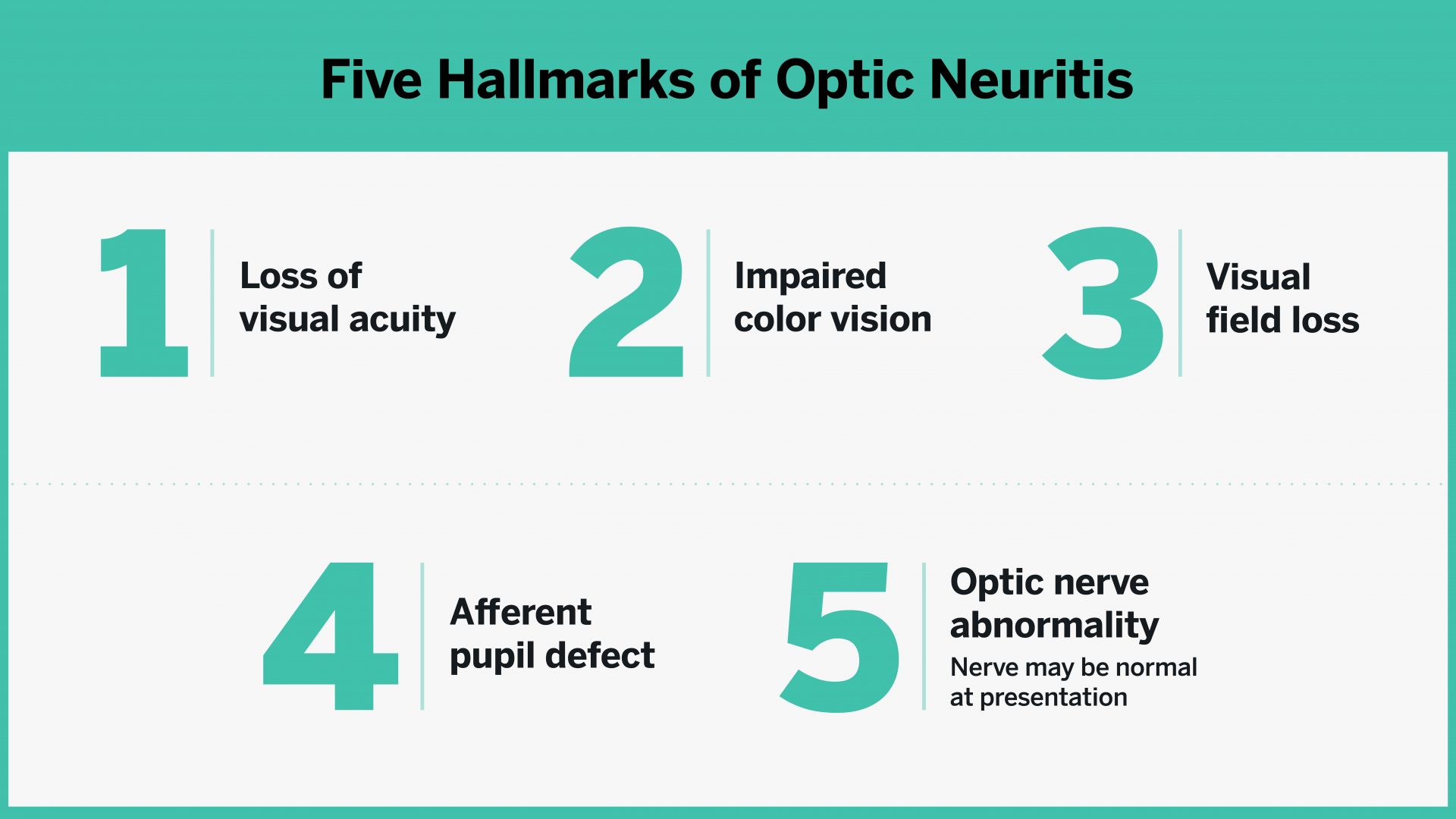
Differential Diagnosis of Optic Neuritis Can Point to Early Multiple Sclerosis
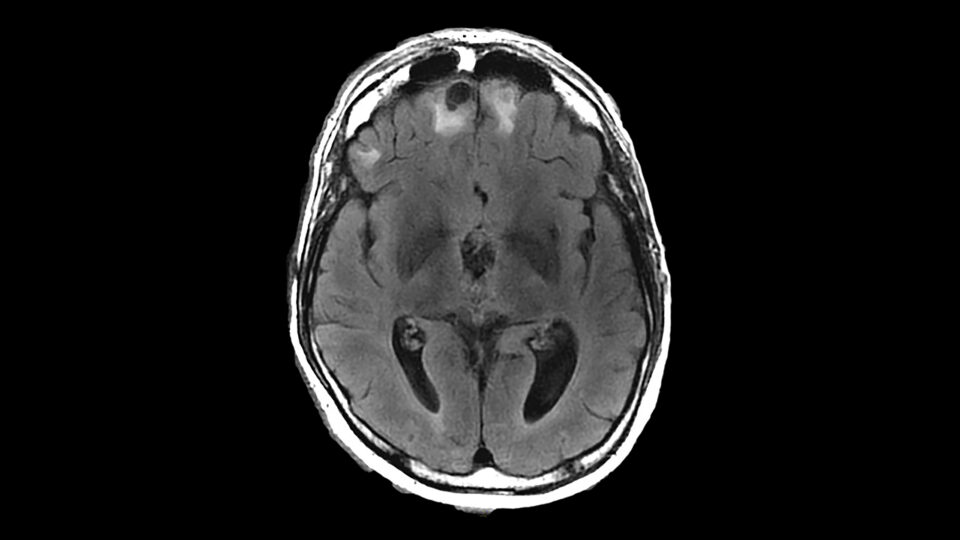
A 24-year-old woman presented with blurred vision that had developed over several days. The woman’s symptoms worsened when her left eye was closed, while her vision normalized with her right eye closed. She reported pain, mainly in the right globe, when she moved her eyes. MRI showed an enhancing lesion of the affected optic nerve and an additional non-enhancing lesion in the periventricular area.
In an invited response to the theoretical case vignette published by The New England Journal of Medicine, NYU Langone neuro-ophthalmologist Steven L. Galetta, MD, concluded that the patient’s features were consistent with demyelinating optic neuritis, an early manifestation of multiple sclerosis (MS) in up to 25 percent of patients. Given the effectiveness of new medications, he responded to the hypothetical case by urging the initiation of disease-modifying strategies to help prevent future attacks.
“The data are now there for giving optic nerve lesions equal footing with the other lesion sites in the diagnostic criteria for MS.”
Steven L. Galetta, MD
Although optic neuritis has long been associated with MS, it has yet to be formally included in the consensus diagnostic criteria of lesions in at least two of four locations within the central nervous system. Dr. Galetta, however, has led a growing effort to prove the utility of optic neuritis as a fifth lesion site in establishing an early diagnosis and therapeutic intervention.
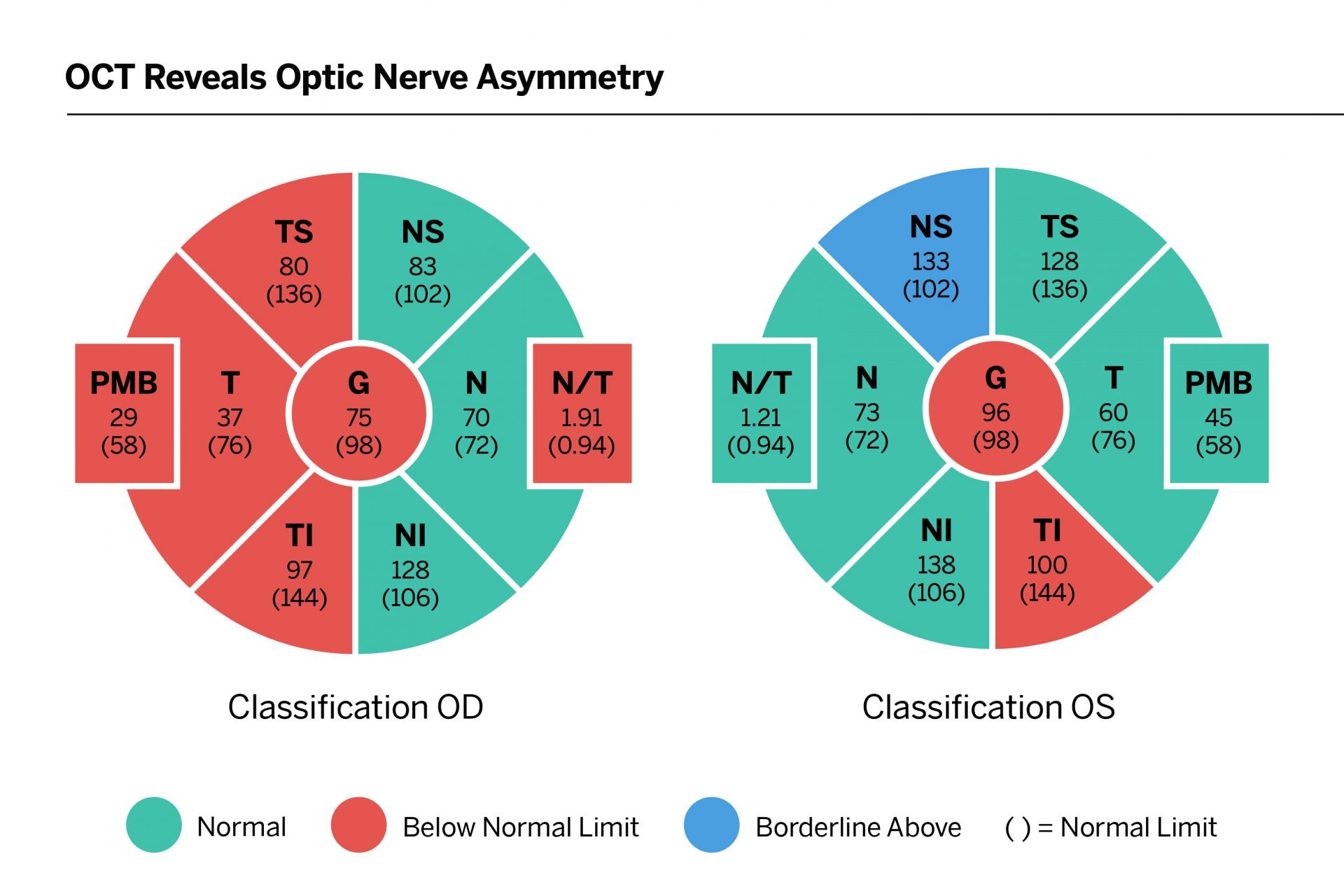
“Our part was in establishing this new technology, optic coherence tomography, to measure the thickness of the optic nerve and validate it as one of the tools you could use to measure optic nerve dysfunction in MS,” he says.
In a widely-cited 2019 study, he and collaborators used optic coherence tomography (OCT) to define the criteria for establishing optic nerve dysfunction in the setting of MS. Multiple studies have since shown that via clinical findings or imaging techniques such as MRI or OCT, including the optic nerve improves the diagnostic accuracy for MS. “The data are now there for giving optic nerve lesions equal footing with the other lesion sites in the diagnostic criteria for MS,” he says.
The promising studies have led to a new editorial in Neurology in which Dr. Galetta and a collaborator at University College London lay out the argument for including the optic nerve in an upcoming revision of the consensus diagnostic criteria and providing what they hope will become a critical new tool for clinicians. Its title references the raft of new evidence: “Assignment Completed: The Optic Nerve Should Graduate to be the Fifth Lesion Site for the Diagnosis of Multiple Sclerosis.”