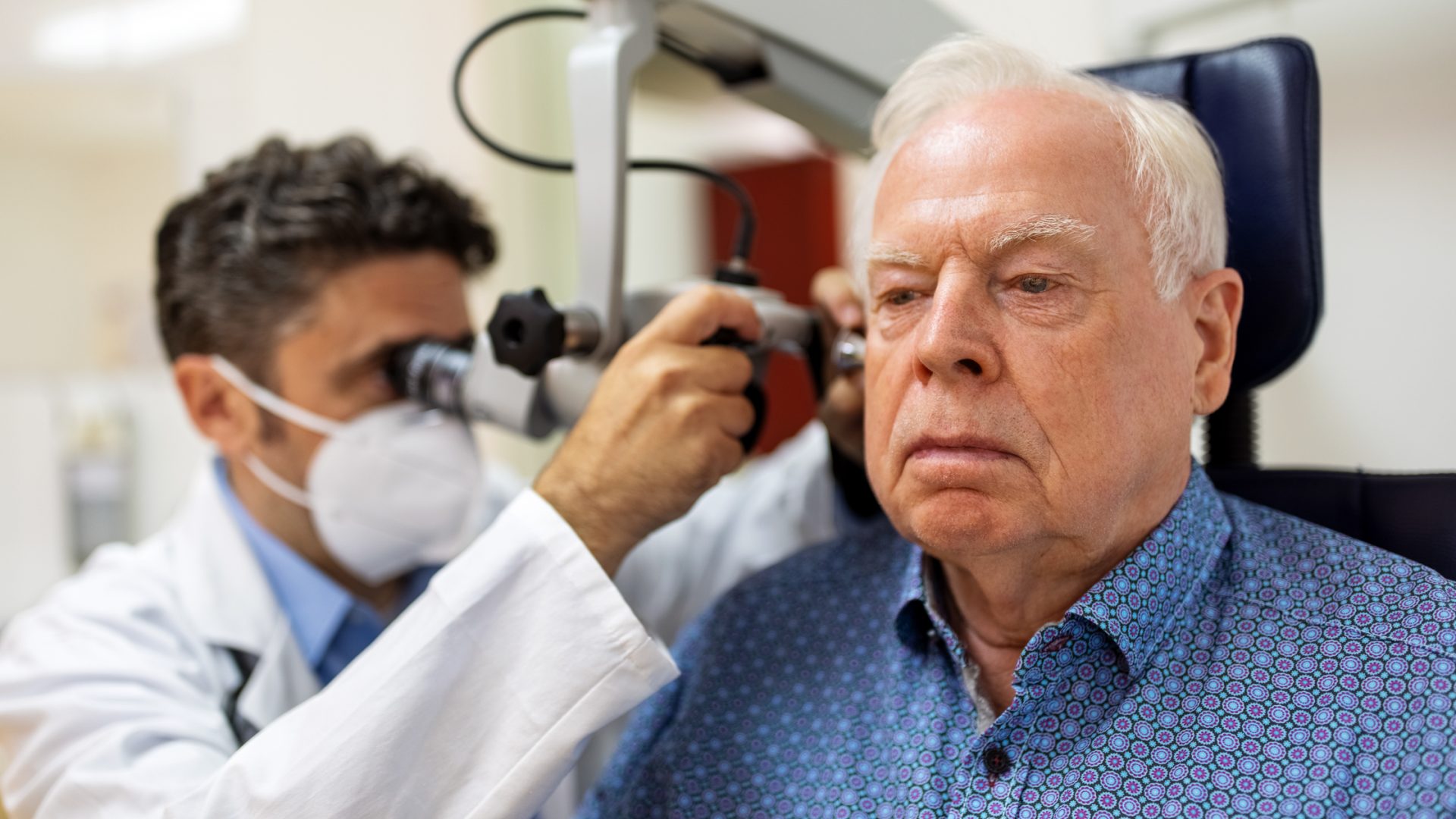
Hearing loss has a significant impact on the health and quality of life of more than 30 million U.S. adults. Among veterans, it is one of the most common service-related disabilities related to military noise exposure.
For those with severe hearing loss, the Veterans Affairs (VA) healthcare system offers comprehensive services, including hearing aids and cochlear implants, that differ from those available to Medicare patients. Cochlear implants can restore speech understanding in patients with severe hearing loss who experience life-changing difficulties such as loss of oral communication and have limited benefits from hearing aids.
To date, there has been little research to clarify the factors influencing how and why veterans and their providers adopt certain technologies for severe hearing loss. David R. Friedmann, MD, an associate professor of otolaryngology—head and neck surgery, is now leading NYU Langone Health researchers in exploring this question using unique databases within the VA system.
“The VA is an optimal setting to study management of severe hearing loss due to unique access to data within the audiometric repository, which allows for identification of patient, system and provider factors associated with receipt of various treatment strategies,” says Dr. Friedmann. “Our long term goal is to confirm evidence-based treatments are available to those most severely affected by hearing loss.”
“Our long term goal is to confirm evidence-based treatments are available to those most severely affected by hearing loss.”
David R. Friedmann, MD
The Pilot Study
Dr. Friedmann and his team are conducting a pilot study of hearing loss, funded by the VA Health Services Research and Development Service, that incorporates video interviews with key stakeholders, including veterans’ primary care providers and audiologists, along with quantitative data from the VA’s robust audiometric and prosthetics database.
“Optimal management of hearing loss requires a good understanding of the perspectives of various stakeholders,” says Dr. Friedmann. “Our multilevel analysis of the longitudinal VA dataset will allow for the identification of both the macro- and micro-level factors that impact patient care.”
This mixed methods analysis will be used to clarify the prevalence, modes of treatment, and time to treatment of veterans with severe hearing loss, as well as identify factors associated with different treatment approaches.
The researchers also plan a thematic analysis of semi-structured interviews to identify barriers and facilitators to particular treatment modalities.
Hypothesizing Contributing Factors
Despite guideline recommendations, cochlear implantation in the U.S. remains underutilized, with some studies estimating 6 to 10 percent usage among potential candidates.
While the precise reasons for cochlear implant underutilization remain unclear, experts believe that limited knowledge of candidacy criteria by primary care providers, poor patient understanding of outcomes, and disparities in reimbursement may be contributing factors. This project, Dr. Friedmann says, will be able to explore these and other factors using a repository containing hundreds of thousands of audiograms.
“Delays in implantation can prolong patient disability and may limit successful outcomes.”
“Delays in implantation can prolong patient disability and may limit successful outcomes,” says Dr. Friedmann. “Understanding and addressing these barriers could represent a modifiable risk factor for eligible candidates.”
Changing Patient-Provider Behaviors
Ultimately, Dr. Friedmann believes that the delivery of optimal hearing care requires tailored treatments offered on the basis of specific degree of hearing loss and individual patient preferences within both the VA and civilian population.
Education will also be key, for both patients and providers, Dr. Friedmann notes. “We hope our data will inform the development and testing of educational materials to achieve best practices in the treatment of this condition.”