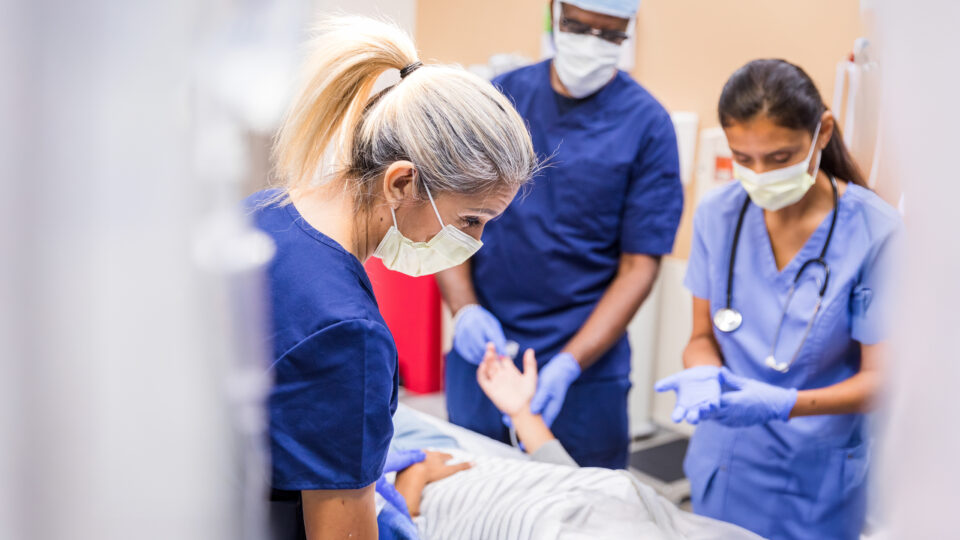
Geriatric trauma patients presenting in the emergency department are at high risk for complications and mortality during hospitalization and less likely to be discharged home. In a pilot program funded by a grant from The Fan Fox and Leslie R. Samuels Foundation, NYU Langone Hospital—Brooklyn will comprehensively examine the geriatric trauma care experience.
“We are looking at those geriatric patients with serious traumatic injuries and trying to develop innovative solutions to provide better care in a complex and vulnerable patient population.”
Lauren A. Parker, MD
“We are looking at those geriatric patients with serious traumatic injuries and trying to develop innovative solutions to provide better care in a complex and vulnerable patient population,” says Lauren A. Parker, MD, medical director of geriatric medicine and palliative care at NYU Langone—Brooklyn. “This program establishes a purposeful process that in and of itself should ensure a higher level of care quality.”
“Geriatricians, and geriatrics as a specialty, have worked hard to improve the inpatient experience for older patients,” says Joshua Chodosh, MD, director of the Division of Geriatric Medicine and Palliative Care at NYU Langone Health. “The Brooklyn program will help to ‘bake in’ new strategies so that the geriatric population can be cared for in a certain way, with greater reliability.”
Steps to Improve Geriatric Trauma Care
Since 2019, geriatric specialists at NYU Langone—Brooklyn have played a robust role in acute trauma care, supporting the trauma service as they navigate core issues for elderly trauma patients such as frailty, delirium, and dementia.
Led by Dr. Parker, the new program, called “Beyond Hospital Doors—Aging Wisely,” will expand the approach to further integrate emergency medicine, trauma, geriatrics, social work, nutrition, nursing, physical therapy, and pharmacy. “We have built a solid infrastructure to ensure this integration happens predictably,” she says.
Focused meetings will be held with all clinical stakeholders to discuss how to collectively care for geriatric trauma patients. A weekly interdisciplinary work group including geriatrics, social work, physical therapy, and trauma will identify barriers to home discharge and formulate new care solutions.
“We want to be sure the right kind of information is transmitted, and the right kind of actions can be taken,” Dr. Parker notes.
Returning Patients to Pre-injury Living
The 18-month pilot program aims to increase discharge to home by 10 percent, reducing transfer to skilled nursing. The hope is that with increased support, patients will be able to resume normal activities with greater ease and independence post-hospitalization.
Another aim is to minimize polypharmacy by decreasing the number of medications or frequency of medication use—removing any medications that cause cognitive impairment.
To reduce barriers to care, social workers will identify family and social support networks that can aid in healthcare decisions. The trauma team will initiate documented advance care planning discussions within 48 hours of admission and identify the need for further social work involvement. Transitional care management will be expanded for patients without primary care physicians or those who cannot see a primary care physician within two weeks.
The program will increase early physical therapy and nutrition consults. Additionally, it will connect patients with services in the community that address vulnerabilities such as food insecurity and other social variables influencing health.
“It’s been very rewarding to see the collaboration among the different departments here at NYU Langone Hospital—Brooklyn, and to establish a more interdisciplinary model of care,” Dr. Parker says. “Everyone is working hard to see how they can improve care of these patients.”
The Groundwork for Change
According to Dr. Chodosh, the program is an opportunity to establish best practices and structures so that even in the absence of a large geriatric care workforce, clinicians elsewhere on the front lines can still “do the right thing.”
“If we do a good job of clarifying the actions that yield the most benefit and how to achieve those actions, it will enable those who aren’t trained in geriatrics to focus on key principles, key issues, and key approaches to ensure we have the best outcomes for this population,” he says.