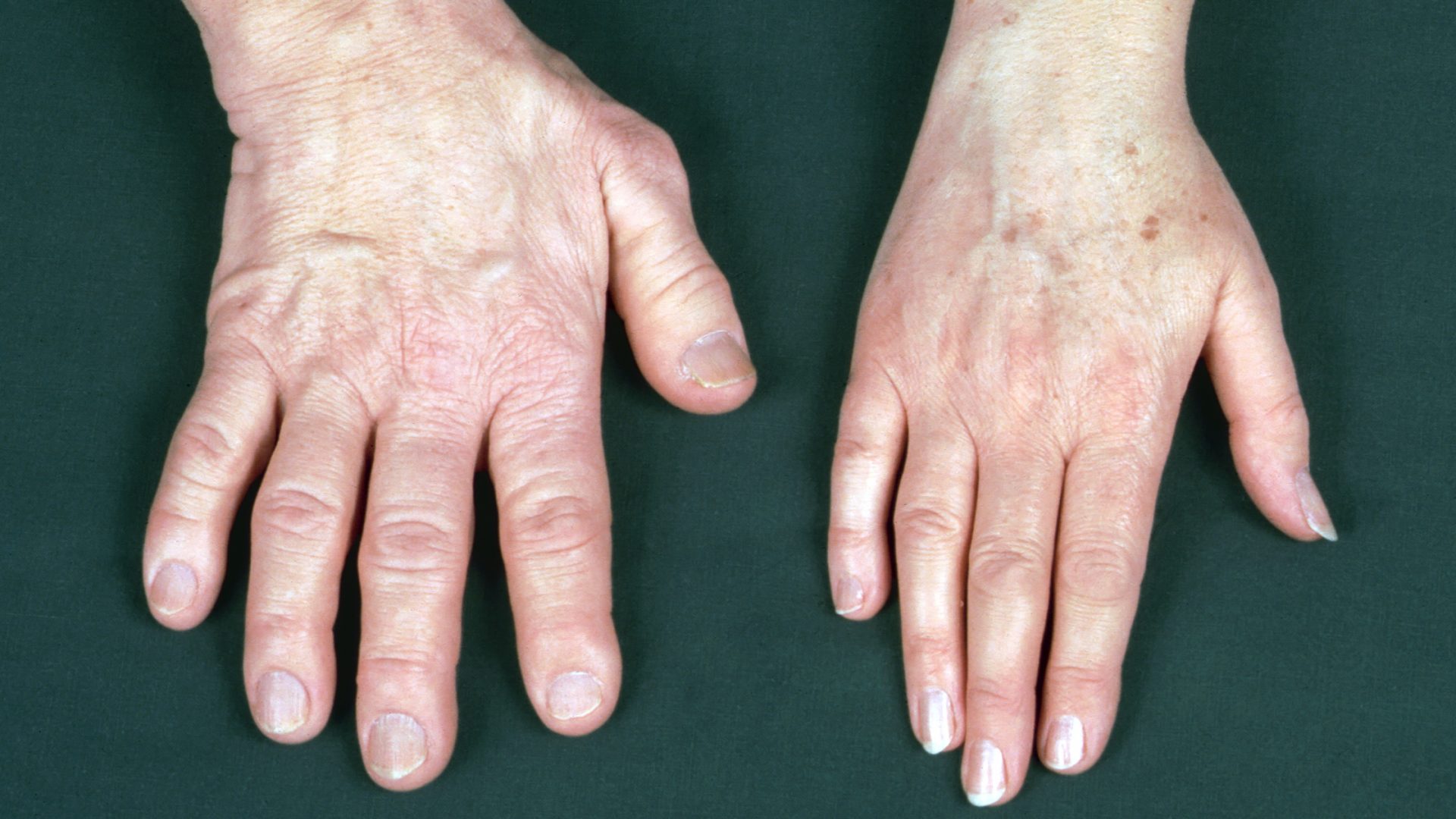
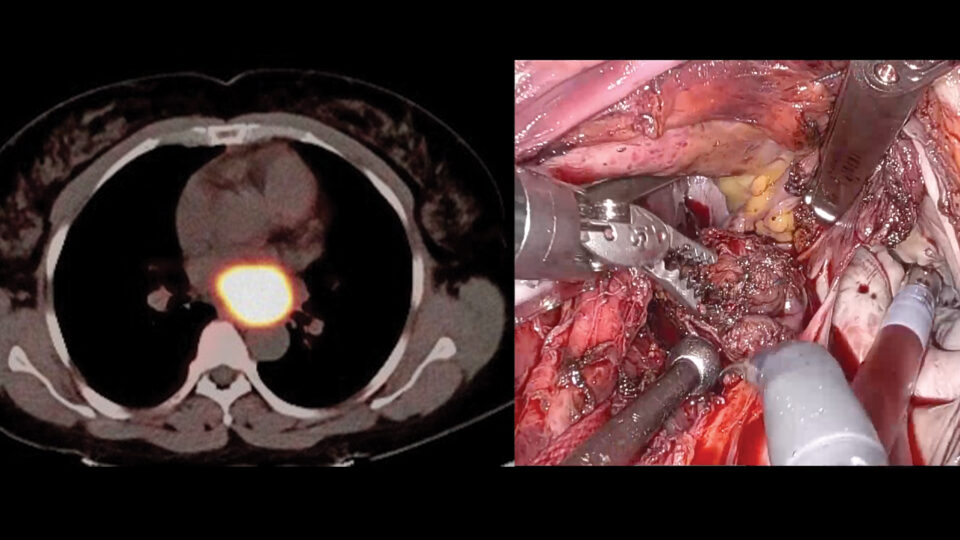
Investigators at the Pituitary Center, including Nidhi Agrawal, MD, director of pituitary diseases, are focused on reducing the gap between symptom onset and management of acromegaly.
As time to biochemical control is a main determinant of morbidity and mortality, Dr. Agrawal says minimizing management delays would go a long way toward improving outcomes for this rare disease.
One product of this effort—a literature review co-authored by Dr. Agrawal—reports that cavernous sinus invasion, large tumor size, and high growth hormone levels are predictive of incomplete remission following tumor resection. Published in Pituitary, the findings may help propel a more personalized approach to patient care for this rare disease.
“While surgery is largely curative, about 40 to 50 percent of patients with acromegaly require the continued support of medication for the rest of their lives,” Dr. Agrawal says. “The question is: Which medication is the best for a certain patient?”
Predictors of Poor Surgical Remission
To determine factors predictive of remission, the researchers identified 77 publications describing outcomes of transsphenoidal selective adenomectomy. Most represented single-center, retrospective studies.
Cavernous sinus invasion arose as the strongest preoperative predictor of poor surgical remission, followed by high growth hormone levels. “Aggressive tumors or those that had bony invasion almost always required medical therapy post-surgery,” Dr. Agrawal explains.
In contrast, low levels of growth hormone in the postoperative period were a robust predictor of durable remission.
These and other prognostic factors, Dr. Agrawal notes, could be incorporated into machine learning models for predicting incomplete response to surgery, which could be used to minimize delays in medical management and further personalize post-surgery treatment.
Optimizing Medical Management
While currently, it can take months for a particular medication to be deemed ineffective and treatment to be modified, Dr. Agrawal and colleagues are pursuing ways to more precisely understand which patient groups are likely to respond to a given therapy.
Toward this goal, the team is helping enroll patients in the national Chiasma Management of Acromegaly (MACRO) registry—the first registry for acromegaly in the U.S.—which aims to develop new oral therapies for patients experiencing challenges with exisiting treatment options.
“It’s all about customizing the medications to the patients. That is where treatment for acromegaly is headed.”
Nidhi Agrawal, MD
“Because all the tumors in acromegaly behave differently, it’s all about customizing the medications to the patients,” Dr. Agrawal says. “That is where treatment for acromegaly is headed.”
Improving Early Diagnosis
The researchers note that patients with acromegaly commonly experience symptoms for five to 10 years before finally being diagnosed with a pituitary tumor. To improve diagnosis, Dr. Agrawal also spends time educating other providers on the slow, insidious onset of the disease.
“The sooner you pick up the disease, the better the outcomes, and for that, education is key.”
As the subtle symptoms of acromegaly include carpal tunnel syndrome, sleep apnea, and dental anomalies, Dr. Agrawal says many of her referrals come from neurology, pulmonology, and dentistry.
“The sooner you pick up the disease, the better the outcomes, and for that, education is key,” Dr. Agrawal says.
In addition, NYU Langone Health has hosted a well-attended, virtual Acromegaly Patient Education Day to help patients with acromegaly, their family and friends learn more about the condition.