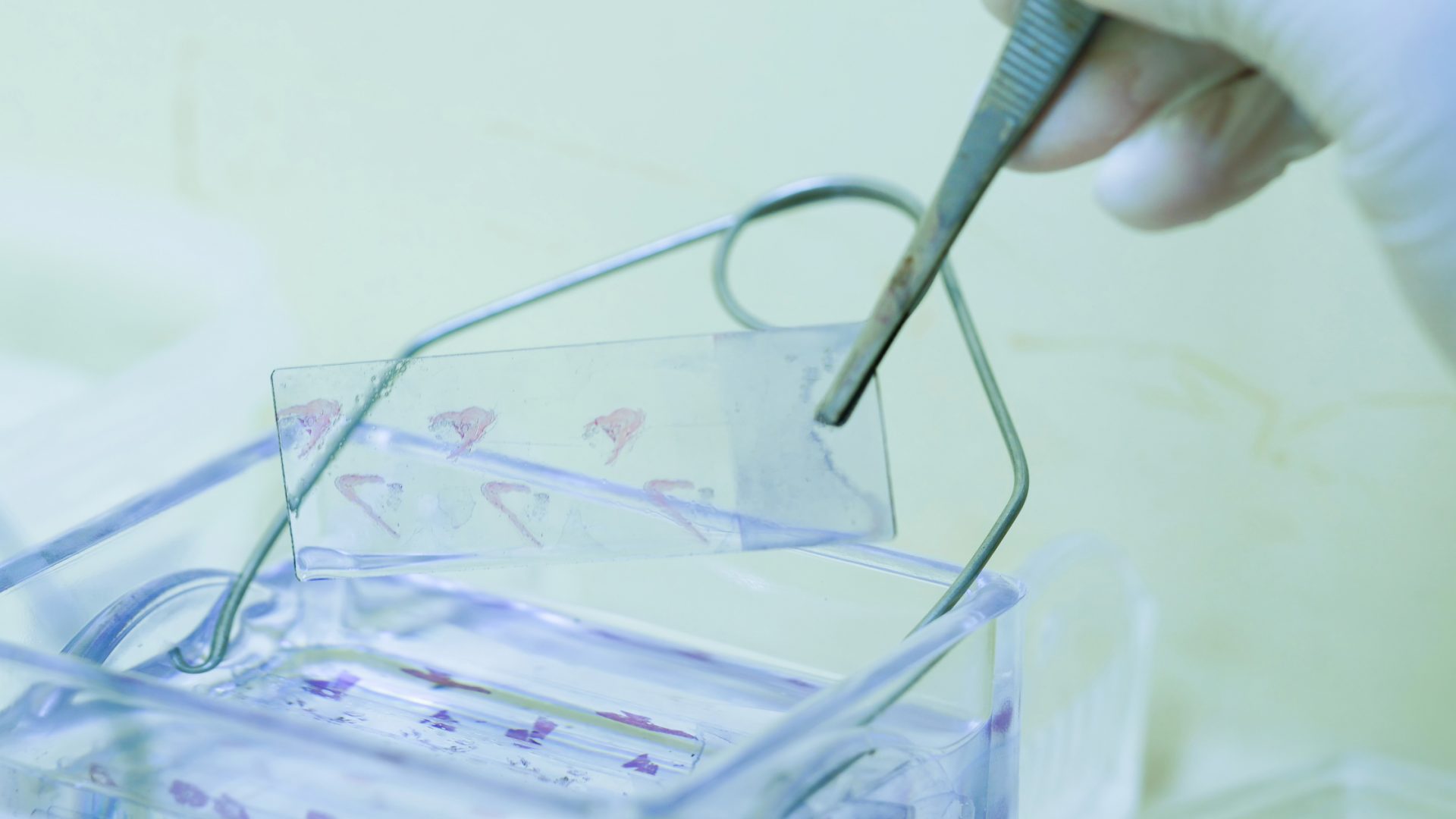
Current techniques for evaluating small bronchoscopic biopsies on-site are resource intensive and may compromise the integrity of samples for later analysis.
Jamie L. Bessich, MD, an assistant professor of medicine and cardiothoracic surgery, is working to incorporate stimulated Raman histology (SRH) microscopy, a novel optical imaging modality, into clinical workflows as a means of facilitating real-time tissue assessment.
In collaboration with Invenio Imaging, Dr. Bessich and colleagues are evaluating the feasibility and utility of SRH microscopy in assessing small bronchoscopic biopsy specimens.
“The beauty of SRH is that it renders tissue reusable, allowing thoracic pathologists to conduct additional studies with the sample.”
Jamie L. Bessich, MD
“We want to be able to analyze lung tissue intraoperatively without losing the sample for downstream analysis,” says Dr. Bessich. “The beauty of SRH is that it renders tissue reusable, allowing thoracic pathologists to conduct additional studies with the sample.”
Putting the Tech to the Test
Raman spectroscopy is a common nondestructive imaging technique with several biosensing applications. Investigators at NYU Langone are also applying the approach to improve brain tumor diagnosis.
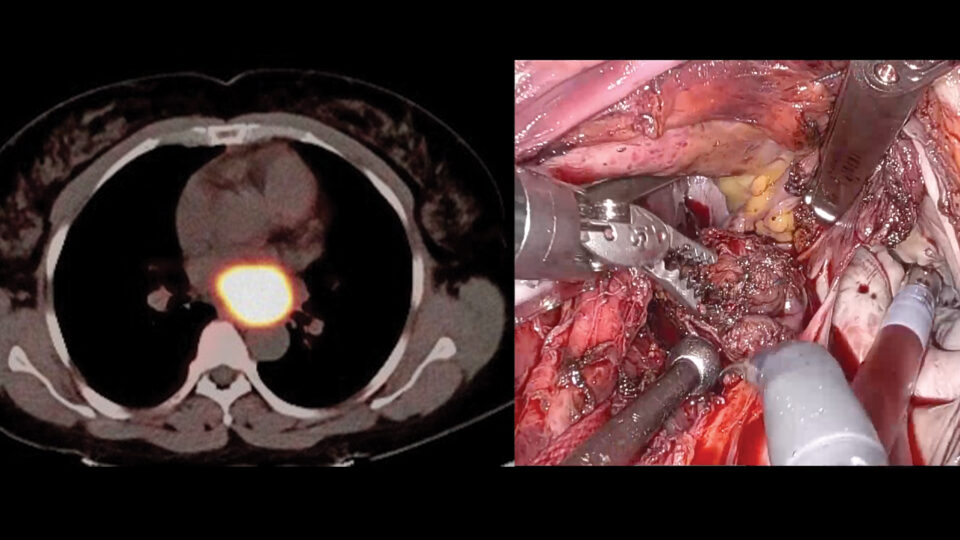
The application of this technology to intraprocedural diagnosis has many potential benefits, including reduced procedure time, decreased total biopsies, and improved yield, and could allow for intraprocedural therapeutics to be applied, especially in cases of peripheral nodules.
“Before our study, the use of SRH was not assesed in lung biopsies,” says Dr. Bessich. “We wanted to know if this technology could enhance the role of the pulmonologist or thoracic pathologist in the diagnosis or characterization of primary lung cancers.”
Dr. Bessich and colleagues imaged specimens using SRH in the procedure room and then submitted them to pathology for fixation and sectioning. After collection, they created a training set of 50 cases from bronchoscopic and surgical lung biopsies.
Subsequently, a thoracic pathologist used this training set to interpret the SRH images, referenced against a surgical pathology hematoxylin and eosin (H&E) image with the final diagnosis. In a prospective validation, the researchers acquired SRH images from 19 cases.
“The samples were imaged sequentially, first with SRH, followed by conventional H&E microscopy,” explains Dr. Bessich. “The 19 prospective cases included a wide range of diagnoses and sample types common in clinical practice, including 6 benign cases and 13 lung malignancies. The thoracic pathologist evaluated each of the 19 SRH case images and provided a diagnosis.”
Promising Results
For the presence of diagnostic, neoplastic tissue, there was strong case accuracy, sensitivity, and specificity, says Dr. Bessich. Furthermore, almost all of the images were considered adequate for diagnosis and downstream analysis.
“These results are a testament to the expertise of the thoracic pathologist who is trained to interpret SRH images, confirming that they have high fidelity for what was observed in the actual specimen,” says Dr. Bessich. “Importantly, however, these data are based on a very small number of cases, and future studies need to be conducted to assess the feasibility of the system on a larger scale.”
Clinical Applications
While the application of this technology to intraprocedural diagnosis is promising, Dr. Bessich and her team believe that clinical use of SRH microscopy could also aid in the selection and prompt delivery of therapy for patients.
“In the clinic, we’re often waiting for weeks to receive molecular results from tissue,” says Dr. Bessich. “If we could obtain these results in real time, we could initiate appropriate therapy sooner.”