Multimodal Imaging Adds Another Layer of Innovation
When the same patient kept presenting to the emergency department with ventricular tachycardia requiring shocks from an implanted defibrillator, Chirag R. Barbhaiya, MD, a cardiac electrophysiologist and specialist in cardiovascular disease, considered all options before his team in the Heart Rhythm Center and radiation oncology decided the case warranted a groundbreaking approach: stereotactic radiation therapy guided by novel, multimodal imaging.
The patient had already undergone several cardiac catheter ablations to prevent the dangerous heart rhythm and reduce the recurrent need for shocks. The ventricular tachycardia stemmed from a prior heart attack, and the area of the heart causing the arrhythmia could not be treated by a catheter-based procedure.
“We were able to figure out exactly where this patient’s rhythm problem was coming from,” Dr. Barbhaiya says. “But because of its location, the energy source we use, and the thickness of the tissue, we couldn’t get enough energy to the area for a successful ablation.”
“It’s a promising therapy for patients that have no other option.”
Chirag R. Barbhaiya, MD
Planning the radiation treatment required an army of specialists all working to pinpoint the smallest area of tissue in the patient’s heart that could be targeted to prevent the arrhythmia.
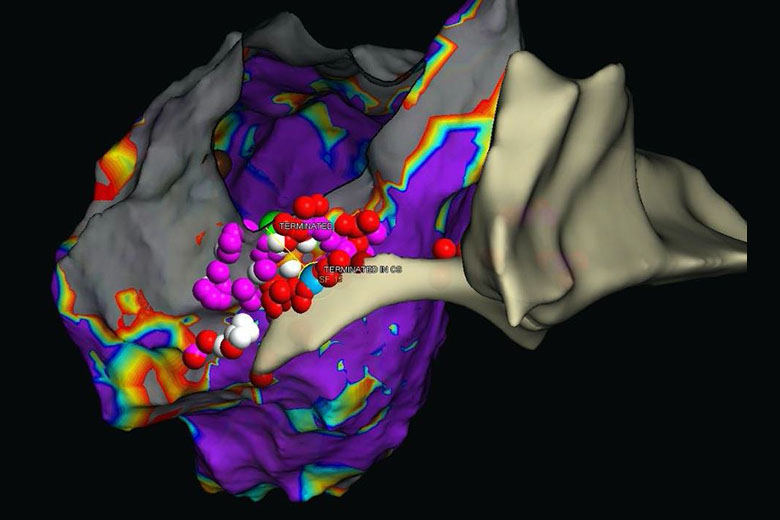
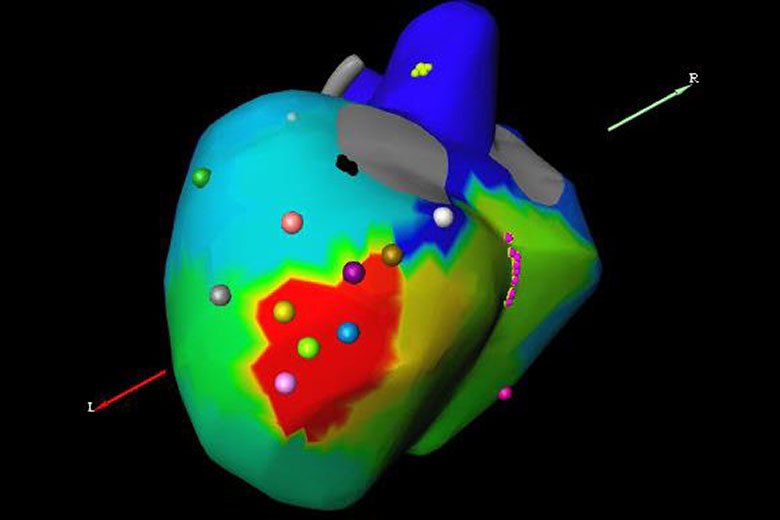
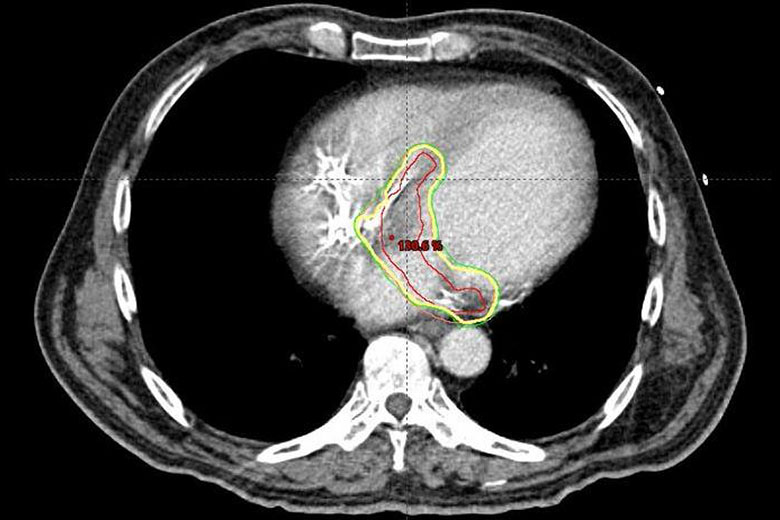
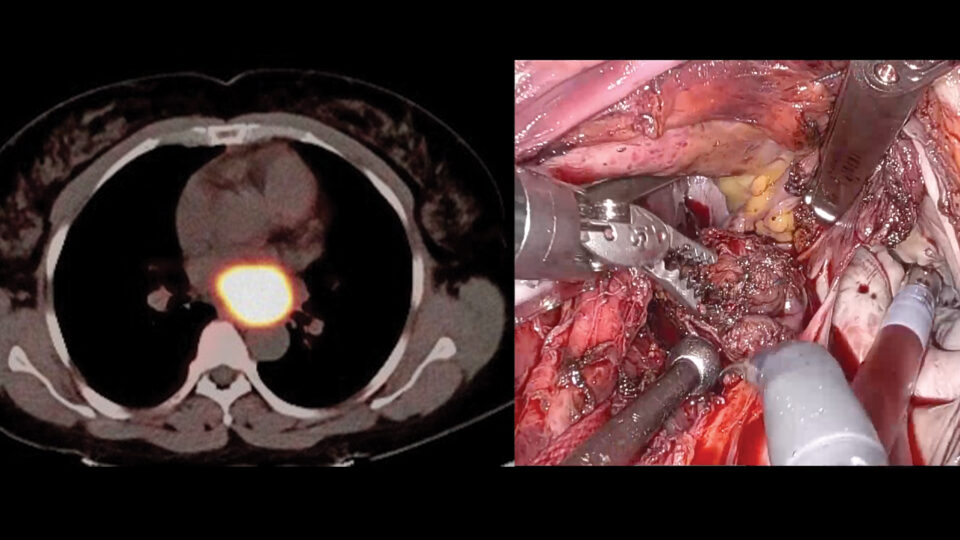
A key element was a non-invasive program stimulation, or NIPS, with non-invasive mapping, a procedure that creates an electrical map of the ventricular tachycardia after the heart is stimulated to recreate the arrhythmia. The patient wears a monitoring vest while an electrophysiologist stimulates the heart via the patient’s defibrillator and tracks cardiac responses.
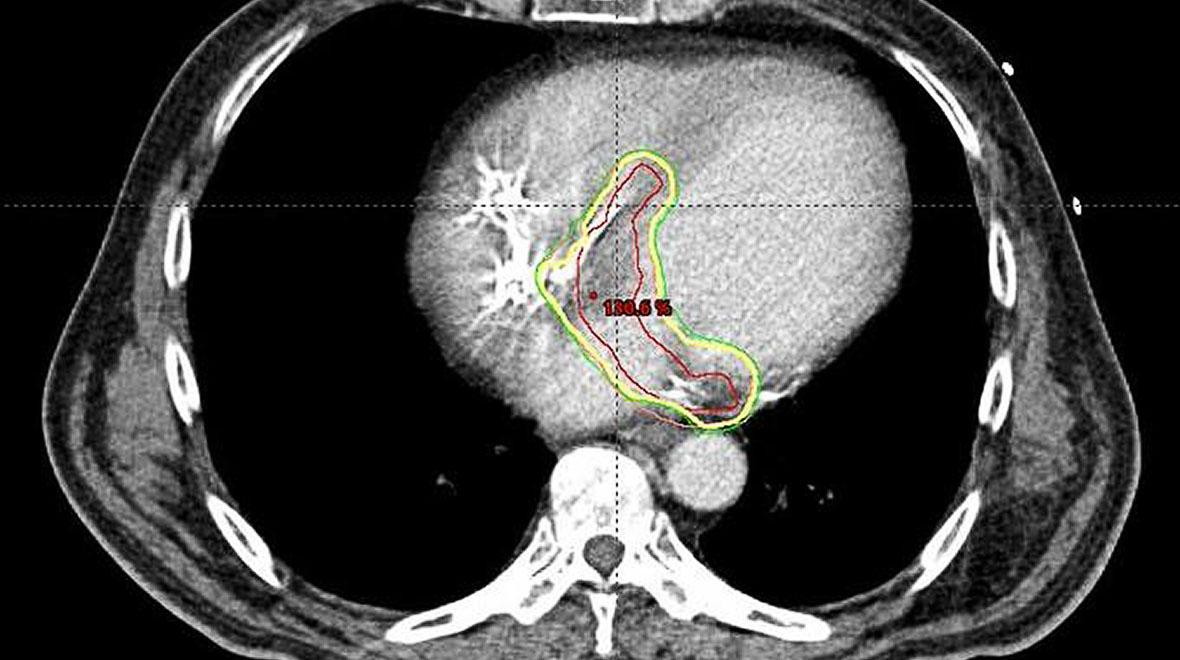
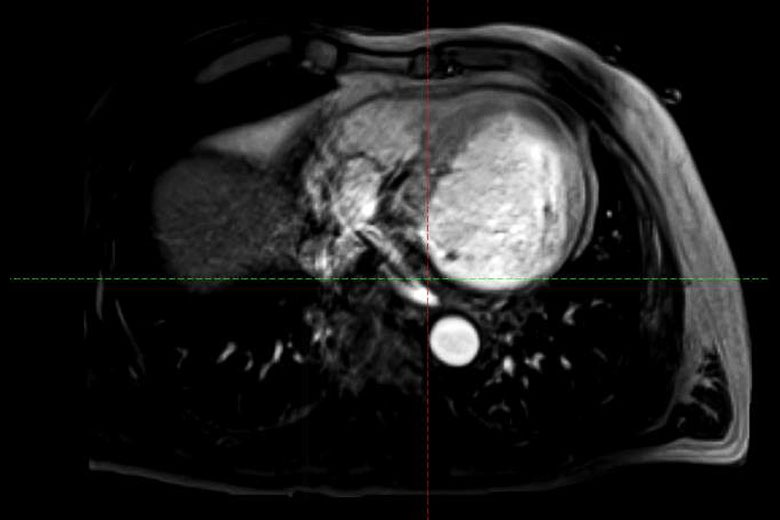
The electrical maps are combined with a cardiac CT scan. Dr. Barbhaiya relied on radiologists, medical physicists, as well as outside consults to evaluate the combined images and determine, within millimeters, the best region and approach for radiation therapy. While the procedure required upwards of a week to plan, the actual radiation therapy was less than 15 minutes.
“It’s clearly very early and the technology is still under development, but it’s a promising therapy for patients that have no other option,” Dr. Barbhaiya says, adding, “Treatment was done on a Friday, and they were discharged on a Saturday.”