At NYU Langone Hospital—Long Island, physiatrist Lincy S. Thadathil, DO, sees most of the patients with concussion who come through the hospital’s emergency department and outpatient office.
A specialist in traumatic brain injury, Dr. Thadathil is part of a multidisciplinary concussion team focused on individualizing treatment. “No two concussions are exactly alike,” she says. “Each patient who walks through our doors is managed a little differently.”
If not detected early and managed properly, concussion can result in prolonged neurologic symptoms, Dr. Thadathil says. At NYU Langone Health, a precise methodology based on leading-edge research in concussion management is used to evaluate the array of concussion symptoms that may affect function.
“No two concussions are exactly alike. Each patient who walks through our doors is managed a little differently.”
Lincy S. Thadathil, DO
“Brain disturbances may not show up immediately, so it’s important to thoroughly evaluate these patients,” Dr. Thadathil says. “The assessment checklist helps us address what actually happened, targeting each subgroup of symptoms—physiological, oculomotor and vestibular, cervical spine, and mood and cognition.
“The goal is to initiate treatment as soon as possible and direct specific rehabilitation when persistent post-concussion symptoms are detected.”
Individualized Rehab
Once the initial evaluation is complete, a rehabilitation plan is developed to manage each symptom individually.
This individualized rehabilitation takes a highly specialized, multidisciplinary team approach, involving experts in vestibular rehabilitation, neuro-focused occupational and speech therapy, neuropsychology, endocrinology, and otolaryngology.
In most situations, patients are managed as outpatients. However, depending on the severity of the injury and symptoms, patients may be evaluated in the hospital.
When the patient leaves the hospital, Dr. Thadathil works with social work and case management to transition them to the appropriate level of rehab—whether at Rusk Rehabilitation or another facility closer to home, either subacute or outpatient.
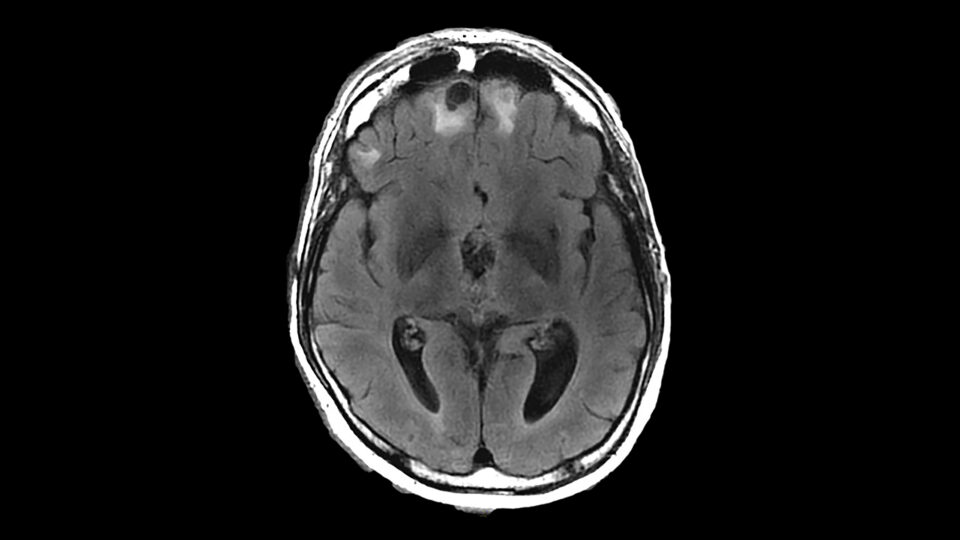
“Most concussions don’t show up on MRI, so we need better methods to measure brain changes sooner, rather than later, when they have already occurred.”
“If they’ve done well with the structural rehab at the hospital, we will help them transition into the community—to their house with home health, outpatient follow-up with me, or medication monitoring and outpatient therapy in the office,” Dr. Thadathil says.
Diligent Monitoring
While most patients with concussion recover within a few weeks, Dr. Thadathil says, a significant group experiences persistent post-concussive symptoms, some of which may be from associated cervical or persistent vestibular dysfunction. She and the rehabilitation specialists monitor each patient’s progress and watch for these post-concussion sequalae that may occur once a patient leaves the hospital or the initial evaluation.
To help patients self-recognize warning signs of concussion and seek care, Dr. Thadathil and colleagues are engaged in community outreach.
“Through our public education, some individuals come in by themselves because they believe they’ve had a concussion, or for a second or third opinion,” she says. “We’re teaching them to identify the symptoms and seek early evaluation.”
Concussion Research
Looking to improve methods for evaluating and monitoring concussion, Dr. Thadathil is participating in a research study led by neuroradiology colleague Yvonne W. Lui, MD, Unpacking the Importance of the Structural Injuries of MTBI. The study will apply new MRI techniques, including advanced diffusion MRI, to measure brain microstructure changes in patients who have sustained concussion in the past six months. The goal is to identify distinct changes associated with recovery outcomes.
Dr. Thadathil and colleagues will also participate in a trial of the Mobile Integrated Cognitive Kit (MICK) in emergency departments. The tablet app was developed by NYU Langone neuro-ophthalmologists to diagnose sideline concussion quickly by assessing visual pathways in the brain.
“Most concussions don’t show up on MRI, so we need better methods to measure brain changes sooner, rather than later, when they have already occurred,” Dr. Thadathil says.