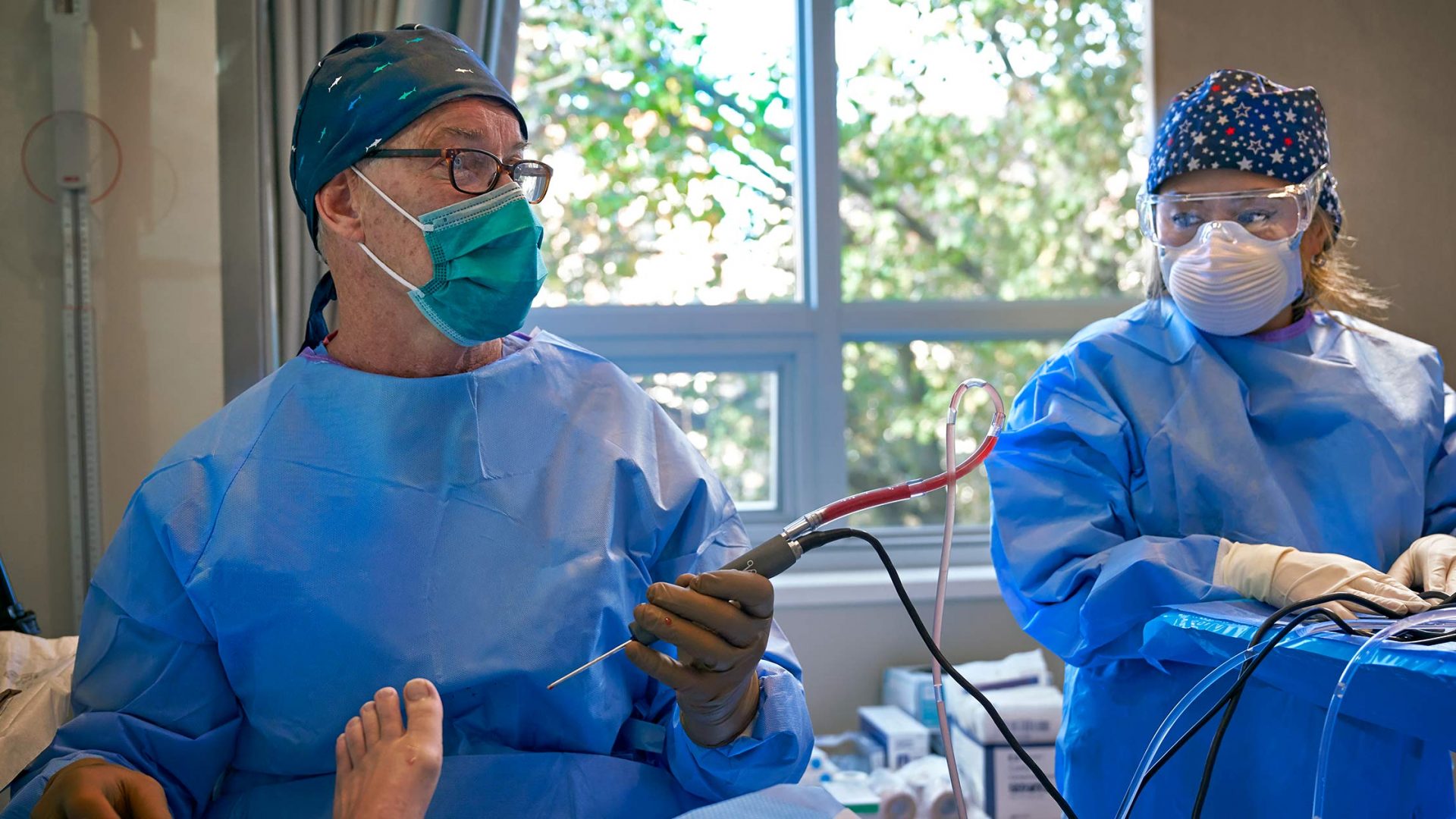
Orthopedic surgeons at NYU Langone Health, led by John G. Kennedy, MD, professor of orthopedic surgery and chief of the Division of Foot and Ankle Surgery, have pioneered a minimally invasive in-office needle arthroscopy (IONA) system, known as NanoScope. Featuring a 1.9-millimeter needle scope and suite of tools, the system is rapidly replacing more involved surgeries and dramatically reducing patients’ return to work and play times.
Dr. Kennedy is now training orthopedic surgeon Arianna Gianakos, DO, under a first-of-its kind IONA fellowship. Here, they discuss the procedure’s promising future.
About the IONA Approach and Its Advantages
Physician Focus: What makes this in-office needle arthroscopy approach so unique?
Dr. Kennedy: IONA is relatively new, and we were the first in the world to use this chip-on-tip technology.
Until recently, there were devices that offered limited visualization, but nobody had the ability to do anything beyond make or confirm a diagnosis. Now, we have a range of 2-millimeter instruments that allow us to repair or replace cartilage injuries and defects, take away scar tissue, and even deliver biologic agents. We can perform procedures in a clinic setting that had previously been done in an operating room, and because the soft tissue trauma is so small, most patients are able to walk off the table afterward.
“We can perform procedures in a clinic setting that had previously been done in an operating room, and because the soft tissue trauma is so small, most patients are able to walk off the table afterward.”
John G. Kennedy, MD
Already, we have published a number of papers showing patient outcomes, including return to play times, are reduced by an order of magnitude in comparison to what we would be doing in an operating room.
Physician Focus: Dr. Gianakos, as the first fellow to be trained formally on this procedure, what are your goals for learning this technique?
Dr. Gianakos: After I completed a year of foot and ankle specialty training at Massachusetts General Hospital, I wanted to further specialize in sports medicine at a leading center in the field. My goal for learning the NanoScope system is to help transfer the technology and training up to Yale. That will also allow us to collaborate with NYU Langone and other top-notch institutions like Yale, Harvard, Amsterdam Medical Center, and Fortius Clinic in London so we can collaborate on future projects and research.
Physician Focus: The NanoScope system allows you as the surgeon to show patients their procedure in real time. What’s the advantage?
Dr. Kennedy: The patient, under local anesthetic, can observe everything and be very much part of the procedure. The result is a much better understanding than if I were to have to explain or draw what I did after a procedure. I can get them to move their ankle or knee and illustrate how things have improved even as we’re doing it. If there’s a divot out of their talus, patients love to see how we’re going in, putting in a scaffold, and adding a biologic to it. The divot’s gone, and now they know because they can see it.
What’s Possible with IONA
Physician Focus: What kinds of procedures are currently possible with this system?
Dr. Gianakos: My initial focus is impingement cases and being able to debride both soft tissue and bony injuries, cartilage injuries. We can also correct osteochondral defects and perform microfracture and biocartilage surgeries.
We’re writing up a report on the technique for ATFL (anterior talo-fibular ligament) injuries that we’ll be presenting at the international ISAKOS Congress. Dr. Kennedy is focused on tendoscopy procedures as well, which is an area in which many foot and ankle fellows don’t get much training in primary fellowships.
Dr. Kennedy: After a more conventional surgery for an ankle sprain, for example, soccer players would be back playing within eight weeks. When patients have an ATFL reconstruction with this device, they’re up and walking within a couple of days, back training within two weeks, and can return to play within four weeks. It’s a massive improvement.
“When patients have an ATFL reconstruction with this device, they’re up and walking within a couple of days, back training within two weeks, and can return to play within four weeks. It’s a massive improvement.”
John G. Kennedy, MD
Physician Focus: Dr. Gianakos, how else has this technology aided your research?
Dr. Gianakos: I’m currently working towards my PhD, which is in gender differences in foot and ankle surgery. Dr. Kennedy has been very supportive and is on a lot of my presentations and research projects, and this technology has helped some things come to light. My hands are a different size than Dr. Kennedy’s hands, for example. How does that impact how the new pen instrumentation and camera fit? I’m also exploring how men and women are responding to watching the surgery and asking questions about it.
Improving Patient Care with IONA
Physician Focus: Where do you see this technique heading in improving patient care?
Dr. Kennedy: Originally, we were doing lots of debridements, but now we have the ability to build as well as remove tissue or debris. We’re building ligaments where we’re putting in scaffolds for cartilage repair and regeneration. For years, the field was delivering biologic agents like platelet-rich plasma or bone marrow or fat in a fairly haphazard way. Now we have precision-guided delivery. We can see where the problem is, see what is the best biologic used to address it, and deliver it exactly where it needs to be.
We are constantly evolving. For instance, we can do a menisectomy and even meniscal repair and labral ligament release here in the office now. We’re minimizing the instrument size so that we can minimize the soft tissue damage or trauma to maximize the patient’s outcome. By doing so, I really feel that we’re heading for the next step: a lot of what we do in an operating room now will not be done there in five years’ time.
Disclosures
Dr. Kennedy is a paid consultant for Arthrex, which produces the NanoScope.